How to write assessment questions for medical affairs training that prepare your team for the field
How do you prepare your medical affairs team for working in the field and at congresses? Without a doubt, much of their time will be spent learning about clinical trials and the evidence they have generated. Whether in eLearning modules or live training sessions, they will be confronted with large amounts of data that they will need to understand thoroughly enough to explain to HCPs.
But MSLs will not get far in the field armed only with percentages and p-values. Their job requires so much more than memorizing and regurgitating data. They need to understand how a study’s design, patient characteristics at baseline, and methods may have impacted both the statistical and clinical significance of the results. They need to be aware of study limitations. They need to avoid overgeneralizing on the one hand and overcomplicating on the other, while never losing sight of hard data underlying conclusions about safety and efficacy.
How your learning materials check and assess knowledge can make a big impact on how well your MSLs can understand and communicate data from your clinical development program. Keep reading to find out how to write effective assessment questions for knowledge checks and activities for your medical training materials.
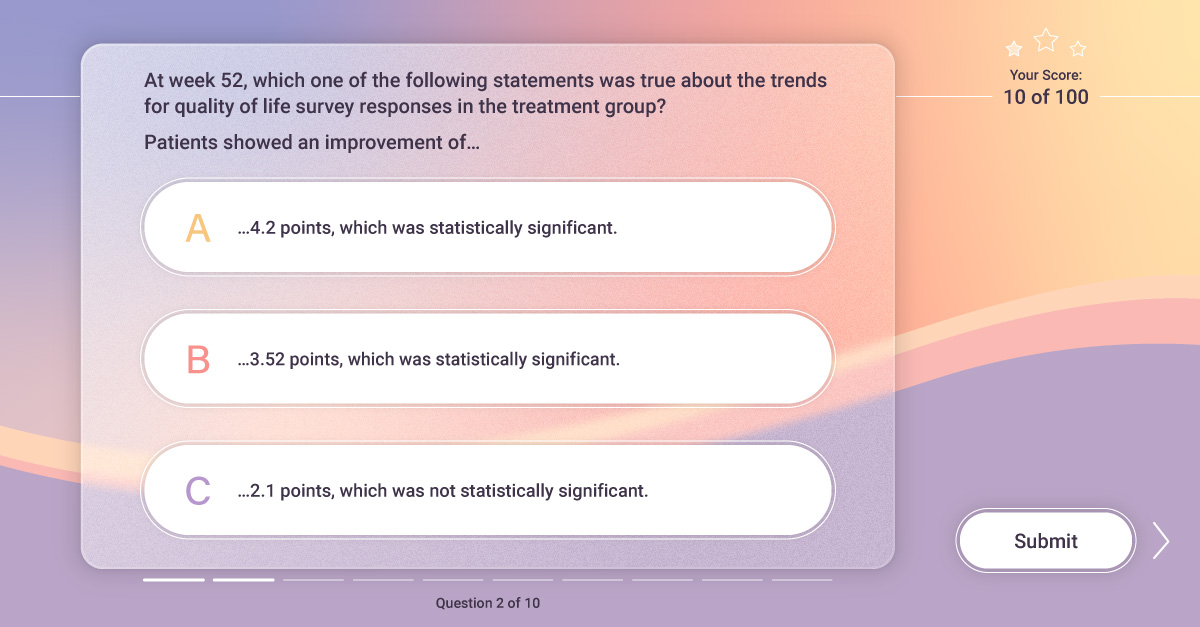
By way of example, let’s take a look at two assessment questions. Both cover the same topic. But they do so in different ways.
Question one focuses on specific improvement values and whether or not those values were statistically significant. Vital information, to be sure. But if the learner does remember the specific values, they are very likely to forget them as soon as they close their laptop. And for their work, they needn’t actually commit those specific values to heart—in the field, they will certainly be presenting the data using a slide deck or an infographic. Most HCPs probably do not expect an MSL to know all of the relevant data points by heart.
More important in this example is whether or not the observed trend was statistically significant. But the way the questions and responses are constructed is flawed: as long as the learner remembers that the result was not statistically significant, they can immediately rule out two of the three responses. And even using basic multiple-choice test-taking principles or guessing, a learner can select the correct response without much trouble. The correct response, after all, is noticeably different from the other two.
Go beyond recall
In contrast, question two is not a simple recall question. It’s a question about the relationship between two factors. The learner has to understand two different aspects of the study and use reasoning to select an answer about the effect one of those aspects has on another. Thinking through the question helps them understand potential weak points in the data, which prepares them for responding to questions and concerns from HCPs.
Assess understanding and not test taking
The learner has to read the options carefully and cannot quickly eliminate them without thinking about the logic of the statements. Someone cannot easily know the answers to these questions without understanding the content presented in the module.
Make the data real
Most importantly, the questions and answers contextualize the clinical trial results presented in the module. They take something abstract—study data—and bring it back to something concrete—how patients responded to a survey to generate data and how researchers collected that data. In this example, many patients had cognitive impairments associated with the disease that could make it harder for them to complete surveys. Understanding the methods on this level is more important than just memorizing specific numbers out of context. If the learner understands this limitation of the study, they will likely also remember that the observed improvement did not meet statistical significance. Understanding the study on this level can help MSLs avoid sloppy generalizations (“quality of life improved”) that can hurt an MSL’s credibility. Assessment questions that promote critical thinking help support transparent medical communication (“the observed improvement was not statistically significant, possibly because some patients may not have fully understood the survey”). This, in turn, builds long-term trust with HCPs.